
Laparoscopic Colorectal Cancer Surgery:
Diagnosis of cancer is a tremendous burden to anybody. It’s with utmost importance to get adequate treatment and support as soon as possible. Colorectal cancer is a cancer of the bowels. A multidisciplinary team of gastroenterologists, oncologists, radiologists, and surgeons should work together to best manage those cases.
From a surgical point of view, there was a substantial change towards minimal invasive techniques over the years and now almost all cancer patients can benefit from it. Laparoscopic surgery /also known as keyhole surgery is now the gold standard in colorectal cancer surgical care and all patients should be offered it over conventional open surgery unless an exclusion criteria exists.
Benefits of Laparoscopic Surgery:
The benefits of laparoscopic surgery are:
- significantly less pain
- quicker return of bowel functions
- decreased mortality
- decreased blood loss
- quicker and easier mobilization
- less chance of wound infection
- less chance of abdominal wall hernia
- shorter hospital stay.
- smaller scars, better cosmetics.
Preparation for surgery:
In preparation for surgery, a Prehabilitation program should bring patients in the best possible condition. As part of it, psychological support from the Laparoscopic surgeon has an important role. Patients should be well aware of what why, and how it will happen, so they can make a well-backed, informed decision.
Nutrition: Healthy, nutritious food rich in protein, energy, and vitamins should be consumed - tailored to the patient’s needs e.g., diabetes, obesity. Proportionate physical exercise will prepare the cardiovascular and respiratory systems (heart and lungs), will modify the metabolic state for good, and will boost the immune system. In my opinion, the effect of such a holistic approach is as important in the successful outcome of an operation as surgery itself.
Expected sequence of events according to my practice:
- Day - 2: Oral antibiotic, liquid food
- Day - 1: Admission to ward, oral antibiotic, oral bowel prep, IV fluid, oral clear fluid, carbohydrate loading
- Day 0: IV antibiotic, carbohydrate loading, surgery, IV fluid, protein-energy drink, mobilization.
- Day 1: Mobilization, liquid food+protein energy drink.
- Day 2: Possible discharge home. If not, same as day 1.
- Day 3: usual day of discharge.
Procedure:
The operation is performed through 3 or 4 small incisions (0.5-1.5cm) and the cancer is removed from the abdomen through a 6-10cm incision, called minilaparotomy.
Colorectal cancer with a segment of bowel and adjacent lymph nodes will be taken and the free ends of the bowels are joined together with stitches or a surgical stapler to restore continuity.
To minimize pain, epidural anesthesia and local anesthesia are applied besides general anesthesia.
In line with Early Recovery After Surgery protocols, early mobilization is encouraged and patients can resume oral feeding on the day of surgery.
In the case of rectal cancer, a diverting stoma - the end of the bowel through which bowel content can empty into a bag attached to the abdominal wall- is sometimes needed, but most often temporary. The need for a stoma can well be predicted and will be discussed beforehand.
The removed cancer will be sent for pathological examination. The result will establish the exact diagnosis and stage of the disease, will guide further management, and can predict long-term outcomes.
Examples of laparoscopy scars and mini-laparotomy 7 days after surgery:
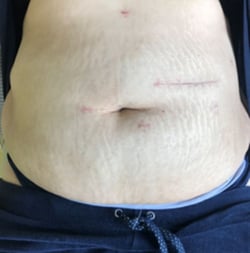
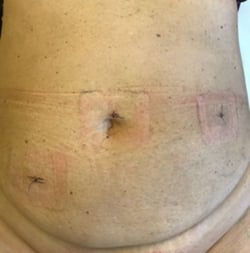
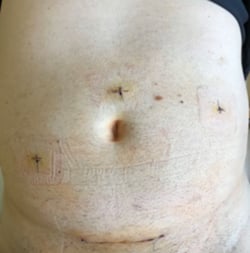
A 78-year-old patient comfortably walked 40 hours after surgery.
Management of colorectal cancer is a complex task requiring a multidisciplinary approach. Laparoscopic colorectal surgery is the cornerstone of treatment offering the possibility to completely remove cancer from the body in the least invasive way.




.png)

.webp)



Leave a comment